Some plastic surgery procedures may be covered by insurance when they are considered medically necessary. These procedures are not performed for cosmetic reasons alone — they are intended to relieve physical discomfort, restore function, support recovery after illness or weight loss, and improve quality of life.
Our Richmond practice works closely with patients seeking insurance-covered procedures such as breast reduction, breast reconstruction (including post-breast cancer reconstruction), gender-affirming top surgery (FTM), and panniculectomy. We help patients understand insurance requirements, determine whether they may qualify for coverage, and guide them through the process as smoothly and clearly as possible. Richmond Aesthetic Surgery accepts insurance from a wide range of providers, including Anthem/Blue Cross Blue Shield, Aetna, Cigna, Humana, Medicare, PHCS, Sentara, Tricare, and United Healthcare.
Schedule a Free 15-Minute Insurance Screening
Speak with a member of our team to discuss insurance coverage, eligibility requirements, and next steps. This brief phone screening is designed to answer initial questions and help determine whether an in-person consultation is appropriate.
During your call, we’ll review the procedure you’re interested in, discuss how insurance coverage typically works, and explain what information may be needed to move forward. You’ll also have the opportunity to ask questions about the process, timelines, and what to expect before your visit. This screening helps ensure your time is used efficiently and that you feel informed and prepared from the start.
Important Notice:
If you schedule a same-day appointment, your insurance benefits may not be fully verified prior to your visit. Our team will follow up as quickly as possible to complete the verification process and review your coverage.
Am I a Candidate for an Insurance-Covered Procedure?
You may be a candidate for insurance coverage if one or more of the following apply:
- Chronic pain or physical discomfort affecting daily life
- Functional limitations related to the condition
- Recurrent rashes, skin breakdown, or infections
- A medical history such as breast cancer or major weight loss
- Supporting medical documentation from healthcare providers
Insurance companies rely on medical criteria, not personal preference, when determining coverage. During your consultation, we will review your symptoms, medical history, and any prior treatments, as well as your insurance requirements. Our goal is to help determine whether you may qualify for coverage and to explain the next steps in the approval process as clearly as possible.
Insurance Pre-Screening & Verification Process
To make the process as straightforward as possible, we offer an insurance pre-screening process designed to provide clarity before an in-person visit. This step helps ensure you understand potential coverage, documentation requirements, and what to expect moving forward.
- Schedule a free 15-minute phone screening
- Securely submit your insurance information
- Our team verifies benefits and eligibility
- Next steps are clearly explained based on your coverage
Our experienced team works directly with your insurance provider to review benefits and determine whether additional information may be needed. This process allows patients to better understand their options, avoid unnecessary surprises, and make informed decisions before proceeding.
Procedures Commonly Eligible for Insurance Coverage
Insurance coverage is determined by medical necessity and documented symptoms. The following procedures are among the most commonly covered by insurance when specific criteria are met.
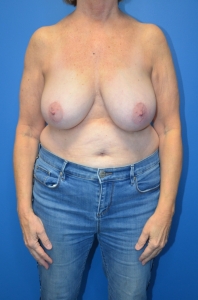
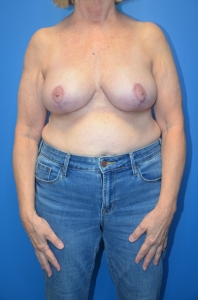
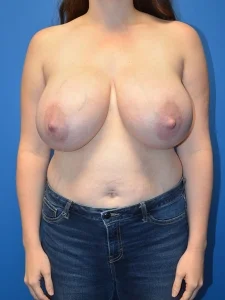
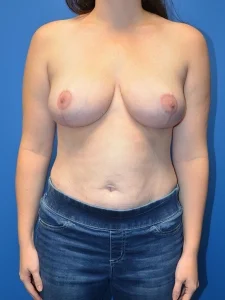
Breast Reduction Surgery
Breast reduction may be considered medically necessary when large breasts cause chronic neck, back, or shoulder pain; bra strap grooving; posture problems; skin irritation; or limitations in daily activities. Coverage typically depends on documented symptoms and required tissue removal amounts.
Gender-Affirming Top Surgery (FTM)
Many insurance plans provide coverage for gender-affirming chest surgery when specific medical and documentation criteria are met. Coverage requirements for FTM top surgery vary by plan and may include supporting letters and a formal diagnosis.
Breast Reconstruction
Breast reconstruction following breast cancer is considered reconstructive surgery and is typically covered by insurance. Coverage may also extend to procedures performed to restore symmetry following reconstruction.
Panniculectomy
A panniculectomy may be covered when excess abdominal skin after significant weight loss causes chronic rashes, infections, hygiene issues, or functional limitations. This procedure focuses on removing medically problematic skin rather than cosmetic contouring.

How Does Insurance Coverage Work?
Insurance companies distinguish between cosmetic procedures and those considered medically necessary. To qualify for coverage, patients must meet specific criteria outlined by their insurance plan, which often includes documentation of symptoms, duration of medical issues, and prior conservative treatments.
Coverage requirements vary widely between insurance providers and individual policies. Our team assists patients by reviewing insurance information, explaining coverage considerations, and outlining next steps once eligibility is determined.
Patient Experiences
Patients seeking insurance-covered procedures often share how meaningful their results have been — not only physically, but in their daily comfort, confidence, and quality of life. Our team is committed to providing attentive, supportive care throughout every stage of the process, from initial screening through recovery.
Dr. Zemmel is hands down the best doctor in Richmond! He is the kindest most compassionate man with amazing skill to match! Everyone at his office is wonderful!
Andrea Feits
January 16, 2018